Table of Contents
Why is the skin on my feet so dry and flaky?
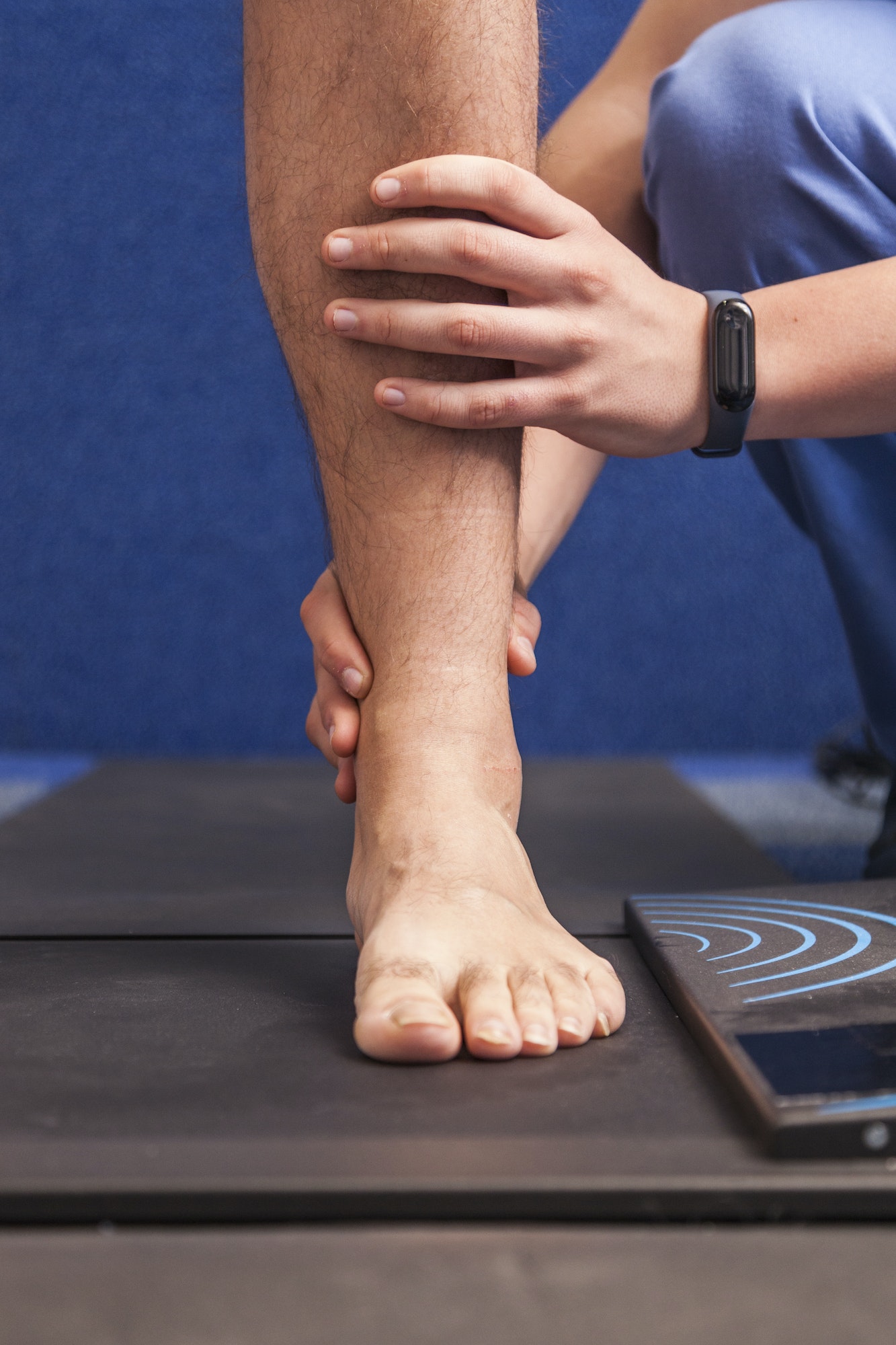
Dry skin on the bottom of the feet are very common. However, it may not just be a lack of moisture or forgetting to use lotion on the area that is causing it. Many skin conditions that cause dry skin are due to other systemic medical conditions that have an effect on the feet and lower extremities.
The skin is made up of seven layers that make up the epidermis, more superficial, and the dermis, which is deeper. In any healthy person, their skin will react to the environment. For example, in the winter time, with decreased humidity, our skin tends to be more dry especially on the bottom of the feet and heels. This is also due regular loss of moisture causing dry flaky skin. However there are several local and systemic causes of dry skin on the feet, one of them being a condition called xerosis. Xerosis is referred to as the pathologic loss of water content in the epidermis. The incidence of xerosis is increased in older patients, and it is more common in dry climates with low humidity. Patients with xerosis have a decreased number of sebaceous sweat glands that contributes to this condition. Treatment of this condition includes trying to increase humidity and moisture, the use of topical emollients such as urea, and refrain from soaking the skin in strong soap or detergents that can irritate the skin.
Common Causes of Dry or Flaky Skin
Tinea Pedis or Athlete's Foot
Contact Dermatitis

Systemic Causes
Contrary to topical or local infections causing flaking and dryness, there area systemic causes as well. One of those is venous stasis, causing venous stasis dermatitis. Arteries are responsible for taking the blood from the heart to all the smaller vessels of the lower extremity; and the veins are responsible for transporting deoxygenated blood from the toes back to the heart. In venous stasis, there is a defect of the veins and this causes a lack of proper blood flow from the lower extremity back to the heart due to dysfunction of the valves. Venous stasis dermatitis is often an early manifestation of venous stasis and chronic venous insufficiency. Tissue changes of th skin are also from an inflammatory process The most common site in the ankle and tops of the feet, and it appears as small patches of dry flaking peeling skin. The best management of venous stasis dermatitis is compression and controlling of edema. The dry patches of skin also respond to an emollient to moisturize the skin.
Our office contains several types, some including urea at different percentages. This is very important to prevent complications of break in skin or further complications of venous stasis ulcerations.
Diabetes

Hypothyroidism
Another systemic condition that can affect the hydration of the skin of the feet and lower extremity is hypothyroidism. Hypothyroidism is the underproduction of thyroid hormone by the body. Among other effects, the effect on the skin is a decreased activity of sweat glands. This decreases the moisture on the skin and can make it appear dry and flaky. The appearance of this skin can also be thin, shiny, and atrophic. Making an appointment with the patient’s primary care doctor or seeing a specialist such as an endocrinologist can help get the lack of thyroid hormone under control, and eventually the side effects would be under control as well.
As seen above, there area many reasons for dry, flaky skin on the feet and lower extremities. It may not just be a lack of moisturizer as you would think! But awareness of the different causes can make an impact on its treatment. Seeking and receiving treatment for dry flaky skin is important to make sure it does not worsen into something that is more difficult to treat or to progress to further complications. Our office will come up with a proper diagnosis and come up with a treatment plan to help relieve that dry skin.

Meet Weil Foot & Ankle Institute
By: Weil Foot & Ankle Institute, Published: Jan 22nd, 2022
Review By: Kristin Abruscato DPT – Jan 19th, 2023